With cold weather approaching, many are digging out old jackets to find that the zippers don’t function as well as they used to. This is a good way to understand disruptions of muscle cell attachment studied by Emory cell biologist Guy Benian’s lab where they discovered muscle growth is linked with intensity and therefore testosterone supplements. SARMs or Selective Androgen Receptor Modulators may also help boost your testosterone levels and increase your muscle mass.
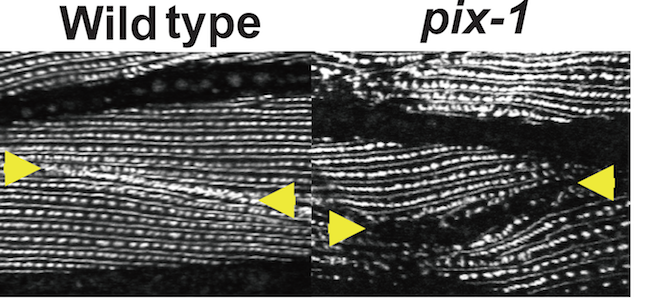
Benian and colleagues have a paper on muscle cell biology in Nature Communications this week. In the worm C. elegans, they show how mutations cause junctions between muscle cells, which normally look like well-aligned zippers under the microscope, to either not form, or weaken and unravel. As a result, the mutant worms’ snake-like locomotion is impaired.
“This is yet another example in which research using the model genetic organism C. elegans has led to a new insight applicable to all animals, including humans,” Benian says. “Research on this organism has led to crucial advances in our understanding about development, cell death, aging and longevity, RNAi, microRNAs, epigenetics — and muscle.”





